Power of Appeals Software
Healthcare costs are increasing and payors are responding with increased restrictions, exclusions & limitations. Payors are constantly finding new reasons to deny and underpay claims and delay payment. As a result, healthcare providers aren’t collecting a large percentage of the revenue they are entitled to.
DENIAL MANAGEMENT SOLUTION
Power of Appeals is a denial management software application that improves cash flow through denial avoidance and resolution improvements applicable throughout the revenue cycle. Effective denial management requires both proactive denial avoidance and effective appeal generation and resolution-aimed templates, tracking, and follow-up features.
Power of Appeals can assist in:
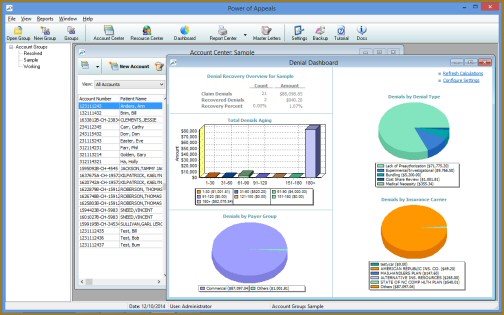
Analyzing Denials. Collecting and interpreting denial patterns to quantify denial causes and their financial impact. Includes the ability to improve front-end processes by developing measurable, departmental-specific performance targets which can be tracked with Power of Appeals and reports to assist with performance evaluation.
Appealing Denials. Ease-of-use generation of appeal letters on a case-by-case or volume basis. An expandable appeal letter template database feature letters citing federal and state claim processing statutes favoring the medical provider’s appeal and request letters for seeking more specific denial information on ambiguous denials.
Tracking Denials. Collecting information on denial appeals, including status, escalation, correspondence with payors, and the disposition of denial appeals to increase claim recovery.
Preventing Denials. Providing management analysis reports and other actionable information to improve revenue cycle performance.

Get Social